Phage to the Rescue
A bacteriophage (virus that infects bacteria) may have cured a patient dying of multidrug-resistant bacteria.
The patient, Isabelle Carnell-Holdaway of Faversham, UK, had a lung transplant, as a result of cystic fibrosis, a condition in which the cilia lining the lungs are paralyzed and bacteria build up. The lung transplant required suppression of the immune system. So a multi-drug resistant bacterium grew and spread throughout her body. The bacterium, Mycobacterium abscessus, is related to those that cause tuberculosis and leprosy—a really nasty pathogen.
But Isabelle’s mother had heard of “phage therapy,” an experimental treatment in which bacteriophages attack a pathogen.

The phages have to be very specific to the bacterial species, which they inject with their DNA to program the cell to make more phage particles. The idea of phage therapy goes way back to the early twentieth century, as dramatized in Sinclair Lewis’s novel Arrowsmith. But no full-scale trials have ever been conducted. There were always antibiotics that worked more simply, and had a broader spectrum of activity.
The problem was, where to find a phage that would specifically infect M. abscessus? Doctors turned to Graham Hatfull, a professor at University of Pittsburgh who has worked with large teams of undergraduates to isolate new phages. This project, which now reaches students all over the world, is called the Science Education Alliance Phage Hunters Advancing Genomics and Evolutionary Science (SEA-PHAGES).

Hatfull searched his collection of ten thousand undergraduate-discovered phages. In the collection he discovered three phages that could attack the specific pathogen that had infected Isabelle. One of the three phages, called Phage Muddy, had been discovered from a rotting eggplant. That gives you some idea of what phage discovery is like.
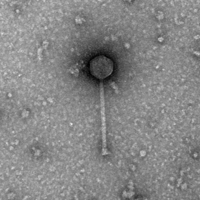
Since no one know which phage would actually work (destroy the infectious bacteria despite Isabelle’s suppressed immune system) she was treated with a combination of all three phages. This was kind of a “Hail Mary” attempt, something you do only when all other treatments have failed.
Isabelle’s infection receded surprisingly fast, then cleared up almost entirely. While the story is not done yet, it looks like phages gave her a miraculous life extension. Time to revisit Arrowsmith.
Comments are closed.


I have “The Forgotten Cure: The Past and Future of Phage Therapy” by Anna Kuchment. While the approach can be very effective, the problem is clearly the slow development of specific phages. To make this work we need libraries of phages, perhaps engineered, that are ready to take off-the-shelf once the bug in question is characterized. This seems daunting today, but perhaps the advent of low cost, rapid gene sequencing of bugs to match with the available phages (using some AI?) may transform this from a niche approach to a mainstream one.
Yes, what is amazing is the large collections of phage that can be screened.
And when you find phage that work, they will be specific to the pathogen, so they won’t hurt the rest of the gut microbiome.
IIRC, Kuchment states that because of anti-biotic supply difficulties, the Soviets were very big on phage therapy.
I wonder if our growing expertise with immune system cells for targeting cancer (and somatic cell gene editing with viral vectors for clinical applications) might be of help in creating and maintaining phage libraries. This technology also requires some painstaking and expensive effort to apply successfully, and so it will also need techniques to have these cells available cheaply on tap. Phages are definitely much closer to “silver bullets” than antibiotics.
If you have access to the BBC iPlayer (UK) via VPN, there is a documentary: “Michael Mosley vs the Superbugs” [[ https://www.bbc.co.uk/iplayer/episode/b08qkz77/michael-mosley-vs-the-superbugs ]. A small section near the end visits a clinic in Eastern Europe where they use phages as an adjunct treatment for A/B resistant bugs. They appear to have phages for specific bugs “off the shelf” although this isn’t clear.
More promising is the technique for growing bugs in their natural environment that appears to show effectiveness at finding bugs that can kill pathogens, promising new antibiotic developments in a 2 decade time frame. There is some suggestion that due to the cost and lack of profitability of antibiotic development, new drugs of this type should be government funded.